Brain Damage in 9 Week Old Babies Due to Lack of Oxygen
Abstract
Background
Extremely depression gestational age newborns (ELGANs) are at adventure of neurodevelopmental impairments that may originate in early on NICU intendance. We hypothesized that early oxygen saturations (SpO2), arterial pOii levels, and supplemental oxygen (FiO2) would associate with later neuroanatomic changes.
Methods
SpO2, arterial claret gases, and FiO2 from 73 ELGANs (GA 26.4 ± i.2; BW 867 ± 179 g) during the first 3 postnatal days were correlated with subsequently white matter injury (WM, MRI, n = 69), secondary cortical somatosensory processing in magnetoencephalography (Million-SII, n = 39), Hempel neurological examination (n = 66), and developmental quotients of Griffiths Mental Developmental Scales (GMDS, n = 58).
Results
The ELGANs with later WM abnormalities exhibited lower SpOtwo and pO2 levels, and higher FiO2 need during the first iii days than those with normal WM. They also had higher pCOii values. The infants with abnormal MEG-SII showed opposite findings, i.e., displayed higher SpO2 and pOtwo levels and lower FiOii need, than those with better outcomes. Severe WM changes and abnormal MEG-SII were correlated with adverse neurodevelopment.
Conclusions
Depression oxygen levels and high FiO2 demand during the NICU intendance associate with WM abnormalities, whereas higher oxygen levels correlate with abnormal Meg-SII. The results may indicate certain brain structures beingness more vulnerable to hypoxia and others to hyperoxia, thus emphasizing the role of strict saturation targets.
Bear on
-
This study indicates that both abnormally low and high oxygen levels during early NICU care are harmful for subsequently neurodevelopmental outcomes in preterm neonates.
-
Specific encephalon structures seem to be vulnerable to low and others to high oxygen levels.
-
The findings may take clinical implications as oxygen is ane of the most common therapies given in NICUs.
-
The results emphasize the role of strict saturation targets during the early postnatal menstruation in preterm infants.
Introduction
Extremely low gestational age newborns (ELGANs), born before 28 weeks of gestational age (GA), are at run a risk of encephalon injury and later neurodevelopmental complications.one,two,3,four,v,6,7,8 Many of these complications are thought to originate during their early on care, when they are exposed to diverse factors, such as oxygen, which is 1 of the well-nigh common therapies given in neonatal intensive care units (NICUs).1,two,7,9,10,eleven,12,13,xiv Inappropriately low oxygen levels are, east.thousand., associated with increased bloodshed and impaired neurodevelopment,9,15,16 and higher levels with retinopathy and lung injury.sixteen Notwithstanding, despite intensive inquiry, the long-term furnishings of early oxygen levels in preterm infants are incompletely characterized.7,10,11,12
Medical data from electronic health tape systems and monitoring devices are increasingly available and methods for analyzing large information sets accept improved, making assay of NICU information system data feasible. As a part of our multimethodological study of ELGANs, nosotros correlated oxygen-related parameters from the start 3 postnatal days of life with neuroimaging (magnetic resonance imaging (MRI)) and magnetoencephalography (Meg) at term equivalent age (TEA) and neurodevelopmental outcomes at two years of corrected age. The main outcomes were white matter (WM) injury in brain MRI and changes in secondary cortical somatosensory processing measured by 1000000-SII, equally these abnormalities may originate during the neonatal phase.viii,17,xviii,nineteen,xx,21,22,23 Neurodevelopmental upshot was assessed by Hempel neurological examination and the Griffiths Mental Developmental Scales (GMDS).
We hypothesized that, in ELGANs aberrant oxygen saturations (SpO2), lower arterial partial pressures of oxygen (pO2), and higher oxygen demand (as measured past fraction of inspired oxygen (FiO2)) during the showtime 3 postnatal days would correlate with pathologic changes in neuroanatomical structures and unfavorable neurodevelopmental outcomes.
Patients and methods
Patients
The original patient grouping consisted of 82 ELGANs, who were born earlier 28 gestational weeks and treated in level Four NICU at Children's Hospital, Helsinki, Finland. They were recruited for a multimethodological study between 5/2006 and nine/2008 and the parents provided signed informed consents. All clinical decisions were fabricated by existing treatment protocols. The SpO2 target range was 90–95%, the claret transfusion range was hematocrit (HCT) <40% when on ventilator intendance and/or needing supplemental oxygen, and HCT <30% for more stable infants. No delayed cord clamping was performed at birth. Six infants died during the NICU menstruation and three infants did non participate in the follow-up examinations. Consequently, the last study population included 73 ELGANs (Fig. 1). The clinical characteristics of the infants are presented in Table 1A, B. The ethics committee of the Hospital District of Helsinki and Uusimaa, Finland approved the study protocols (Dnro HUS 277/E7/2005, 2008 and HUS 115/thirteen/03/00/2014).
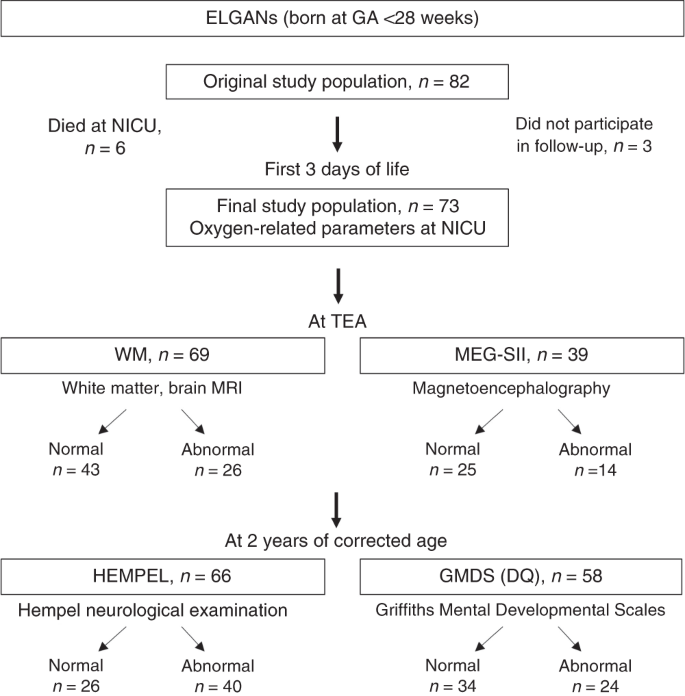
DQ developmental caliber, ELGAN extremely low gestational historic period newborn, preterm babies born before 28 weeks of GA, GA gestational age, GMDS Griffiths Mental Developmental Scales, MEG-SII secondary cortical somatosensory processing in magnetoencephalography, HEMPEL Hempel neurological test, NICU neonatal intensive care unit, TEA term equivalent age, WM white thing, white matter injury in MRI.
NICU biosignal data and oxygen-related parameters
Data gathered during the NICU phase, including patient monitor information, data from ventilators and other medical devices, observation variables, laboratory results, and diagnoses were stored in Centricity Critical Care information organisation (GE Healthcare, Chicago, IL). Monitor and ventilator data including SpO2, FiO2, and heart rate (60 minutes) were recorded automatically and stored every bit 2-min averages of median values for 10-due south intervals. The observation variables include both background information (e.g., GA, mode of commitment, sex activity) and clinical measurements (e.g., SpO2, FiO2). Transmission readings were entered into the database by staff and correspond the value at the time of reading. The partial pressures of oxygen (pOtwo) and carbon dioxide (pCO2) in arterial blood were measured using routine claret gas analyzers.
Brain MRI and determination of WM abnormalities
Brain MRI (1.5 T) including T2-weighted axial and T1-weighted 3D sagittal images was performed at TEA. 2 experienced neuroradiologists classified the MRI images according to Woodward et al. with modifications.17 WM was classified based on five variables: WM bespeak abnormality, periventricular WM volume loss, cystic abnormalities, ventricular dilatation, and thinning of the corpus callosum. The thinning of corpus callosum had two grades (grade i was normal and grade 2 had thinning of the corpus callosum). All the other variables had three grades, grade 1 being normal and grade 3 having nigh astringent abnormalities. Based on the full score, the WM MRI findings were classified as abnormal if the total score was ≥7. In a subgroup analysis, comparisons were performed between patients with normal WM and those with severe WM changes having total scores of ≥10.
1000000 and sensory evoked magnetic fields
MEG analysis was performed at TEA as previously described.eighteen Meg recording was performed using a whole-caput developed-sized helmet-shaped sensor array consisting of 306 independent channels: 204 gradiometers and 102 magnetometers (Vector-view, Elekta Neuromag Oy, Helsinki, Republic of finland). Electroencephalography and electro-oculography were recorded for slumber stage monitoring. The sensory evoked magnetic fields were elicited past tactile stimulus to the tip of the alphabetize finger by a thin rubberband membrane expanded by an air pressure pulse delivered through a plastic tube (Somatosensory Stimulus Generator, four-D NeuroImaging Inc., San Diego, CA) and the interstimulus interval was two southward. The One thousand thousand data were analyzed every bit previously described.18,xix The SII response, peaking at about 200 ms afterwards tactile stimulation, was defined equally abnormal when it was absent after both contralateral and ipsilateral stimulation in at least one hemisphere (right or left).18
Neurodevelopmental assessments
An experienced child neurologist performed the clinical neurodevelopmental assessments at ii years of corrected age co-ordinate to a structured Hempel neurological examination24 and GMDS.25,26 The Hempel neurological examination consisted of five functional domains: posture and musculus tone, gross motor part, fine motor function, reflexes, and visual system. For the present report, infants with any dysfunctional domain(south) were classified as aberrant and the patients with normal findings equally normal. In a subgroup analysis, comparisons were performed between patients with normal Hempel assessments and those with major neurologic impairment (cerebral palsy (CP)).
The general developmental quotient (DQ) of GMDS was based on v subscales: locomotor, personal–social, hearing–language, eye–paw coordination, and functioning. DQ and subscale quotients (SQs) were calculated on the basis of the raw scores and the corrected age of the child. DQ and SQ scores <−1 SD were defined as abnormal and the cutting-off points for harm were for general DQ 88.7, locomotor 84.three, personal–social 84.8, hearing–linguistic communication 84.vi, eye–hand coordination 84.3, and for performance 84.4. In improver to separate SQ analysis, we also compared patients having subscale impairments in either eye–paw coordination or functioning scores or both (abnormal grouping) with patients having normal scores in both these two subscales (i.e., centre–hand coordination and operation; normal group).
Data analysis and statistics
The methods of large data analysis were used, non due to the number of the patients (final due north = 73) but rather due to large and complex NICU database, e.thousand., birthday over million SpO2 measurements. Fourth dimension series data (measurements with associated time stamps) for oxygen-related parameters were extracted from Centricity for Critical Intendance information system and analyzed at the Aalto Academy Department of Computer Science, Espoo, Finland using PostgreSQL database engine. SpO2 and FiO2 data were extracted from data logged automatically via equipment interfaces. Data for pO2 and pCO2 assay came from laboratory information system via Centricity for Critical Intendance information system interface. Supplementary oxygen time series was created past combining automatically logged FiOii from ventilator interface when available (mechanical ventilation, synchronized nasal ventilation) and manually entered FiO2 for patients on nasal continuous positive airway pressure level or loftier menstruum nasal cannulas, where no equipment interface was available. The time serial information were preprocessed by removing out-of-range values caused past, e.k., missing or misplaced sensors and monitoring equipment drifting out of calibration. The data were correlated with WM injury, 1000000-SII abnormalities (both at TEA), and Hempel neurological test and GMDS quotients (at ii years of corrected historic period). Student'south T test was used for statistical comparisons. A p value <0.05 was considered significant.
Results
Patient characteristics
The study design is shown in Fig. 1 and the clinical characteristics of the ELGANs (final n = 73) in Table 1A, B. WM (at TEA) was classified as abnormal in 38%, Million-SII (at TEA) in 36%, Hempel neurological examination (at ii years of corrected age) in 61%, and GMDS quotients in 41% of the patients. These relatively large percentages of infants in the abnormal groups are likely to be explained by the study pattern with classifying infants fifty-fifty with mild alterations in the master abnormal groups. In the subgroup analysis, in that location were 6 infants with severe WM changes (8.7%) and 6 with major neurologic harm in Hempel assessments (CP, nine.1%).
In comparing with infants with normal WM, those with WM abnormalities were more ofttimes males, had trend toward lower Apgar scores, had more oft suffered from respiratory distress syndrome (RDS), and had more intraventricular hemorrhage (IVH) findings in ultrasound examinations (Table 1A). The ELGANs with severe WM changes additionally suffered more from bronchopulmonary dysplasia (BPD) (data not shown (DNS)). The patients with abnormal Hempel neurological examination were more than often males (Table 1B), and the ones with major neurologic impairment (CP) also had more IVH (DNS) than the infants with normal Hempel assessment. The infants with low GMDS scores, in plow, had more retinopathy of prematurity than those with normal scores (Table 1B).
The infants with abnormal WM, MEG-SII, Hempel, or low GMDS did not significantly differ from those without these abnormalities in terms of GA, birth weight, being small for gestational historic period (SGA), being twins, or other parameters shown in Table 1. In improver, none of these groups statistically significantly differed from the other groups in regard to age, parity, and the smoking condition of the mother; existence exposed to preterm premature rupture of membranes, chorioamnionitis, pre-eclampsia, gestational diabetes, cesarean section; being extubated past day 3; or treatment for patent ductus arteriosus (DNS). The infants with abnormal WM and/or Million-SII had tendencies toward having received more postnatal dexamethasone than the ones with normal imaging, merely findings were not statistically meaning (aberrant WM 19% vs normal WM 9%, p = 0.07 and One thousand thousand-SII 14 vs two%, p = 0.09).
Severe WM changes and abnormal Meg-SII were associated with agin neurodevelopment
The severe WM changes at TEA were associated with abnormalities in GMDS and Hempel assessments at two years of corrected age (all p < 0.05, DNS). The aberrant WM grouping that included also minor WM changes was non significantly associated with the 2-twelvemonth neurodevelopmental assessments (GMDS or Hempel, DNS).
The abnormal MEG-SII findings (at TEA) were significantly associated with worse outcomes in 2-twelvemonth GMDS, which is consequent with our previous findings.18 Hither, with a larger study group than in our previous study,18 also the findings with the subscales were statistically significant: the infants with abnormal MEG-SII had significantly lower GMDS SQ scores in locomotor, personal and social, hearing and language, eye–hand coordination, and performance (all p < 0.05, DNS). The patients with abnormal MEG-SII findings tended also to accept poorer Hempel outcomes, although the finding was not statistically pregnant (p = 0.07).
Oxygen saturations and partial pressures of oxygen during the offset three days of life in ELGANs with afterward WM, MEG-SII, and neurodevelopmental abnormalities
During the first iii days of life, the infants who at TEA displayed WM abnormalities showed lower average SpO2 (92.8% ± 0.iii vs 93.8% ± 0.three; p < 0.05. DNS), had more SpO2 <90% (p < 0.05) and <85% (p < 0.05), and less SpO2 >95% (p < 0.05) than the patients with normal WM (Fig. 2a). The cumulative times (percentage of time during the first 3 days) in patients with abnormal and normal WM having SpO2 <85% were 3.5 vs 2.1% (p < 0.05), SpOtwo <ninety% 16.3 vs 12.2% (p < 0.05), SpO2 90–95% 54.1 vs 46.0% (p = 0.06), SpO2 >95% 25.5 vs 38.three% (p < 0.05), and SpO2 >98% 5.8 vs 12.8% (p = 0.06), respectively. Thus, the ELGANs with abnormal WM had spent more time with lower SpOtwo than the infants with normal WM. The subgroup with astringent WM changes showed similar findings and had lower oxygen saturations, i.e., lower average SpO2 and more than SpOii measurements <90% and <85%, equally well as higher cumulative times spent with SpOii <xc% and <85%, than the infants with normal WM at TEA (all p < 0.05, DNS).
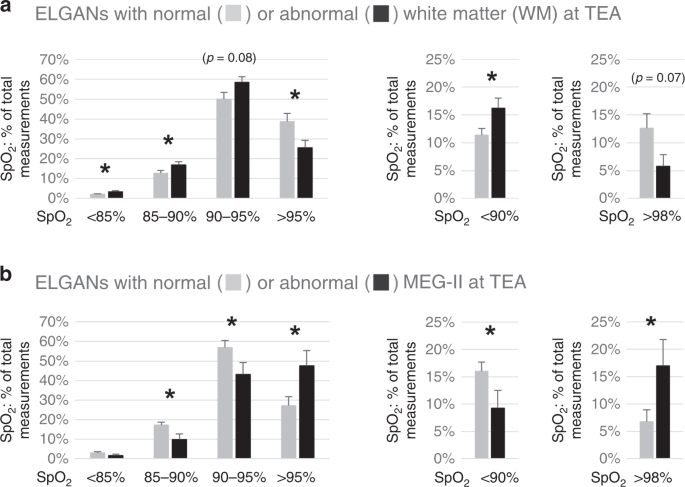
ELGANs with WM changes showroom lower and with MEG-SII abnormalities higher SpO2 than those with normal findings. a SpOii (% of total measurements, mean +/− SEM, *p < 0.05) in ELGANs with normal (due north = 43) or aberrant (n = 26) WM and b normal (n = 25) or abnormal (due north = 14) MEG-SII.
The infants with abnormal Meg-SII, in turn, had higher boilerplate SpOtwo (94.5% ± 0.4 vs 92.viii% ± 0.4 p < 0.05, DNS) and had more SpO2 >95% (p < 0.05) and >98% (p < 0.05), equally well as fewer SpO2 <xc% (p < 0.05), than the patients with normal MEG-SII findings (Fig. 2b). They as well stayed less within electric current oxygen saturation target ranges (ninety–95%, p < 0.05). Furthermore, their cumulative times (percentage of fourth dimension during the first three days) when having higher SpOii (>95% and >98%) were greater. The proportional times (percent of time) in patients with aberrant and normal Meg-SII when having SpO2 <85% were 1.7 vs three.i% (NS), SpOii <90% 9.2 vs 17.vi (p < 0.05), SpO2 xc–95% 40.i vs 51.6% (p < 0.05), SpO2 >95% 47.6 vs 26.5% (p < 0.05), and SpO2 >98% 17.1 vs 6.eight% (p < 0.05), respectively.
The ELGANs with low GMDS SQ scores in eye-hand coordination or performance or both had significantly fewer low SpO2 (i.e., had higher SpOtwo) than their controls with better scores (DNS). The SpO2 levels in other abnormal GMDS subscales did non significantly differ from the ones with normal findings (DNS). The infants with major neurologic impairment in Hempel assessment (CP) had more than SpO2 measurements <85% and higher cumulative times when having SpO2 <85% than the ones with normal Hempel examinations (all p < 0.05, DNS). The oxygen saturations in those aberrant Hempel groups that included also the minor impairments did not significantly differ from the grouping with normal assessments (DNS).
Consistently with the SpO2 findings, the infants with WM abnormalities had lower arterial pO2 levels and patients with abnormal Meg-SII had higher arterial pOtwo levels than the infants with normal WM and Million-SII, respectively, during the first 3 days of life (Fig. 3). Besides, the ELGANs with low SQ scores in locomotor, heart–mitt coordination, or performance had significantly more high and fewer low pO2 levels (p < 0.05, DNS) than the ELGANs with normal scores (DNS). The arterial pO2 levels of the other aberrant GMDS SQs or Hempel examinations did not significantly differ from the ones with normal examinations (DNS).
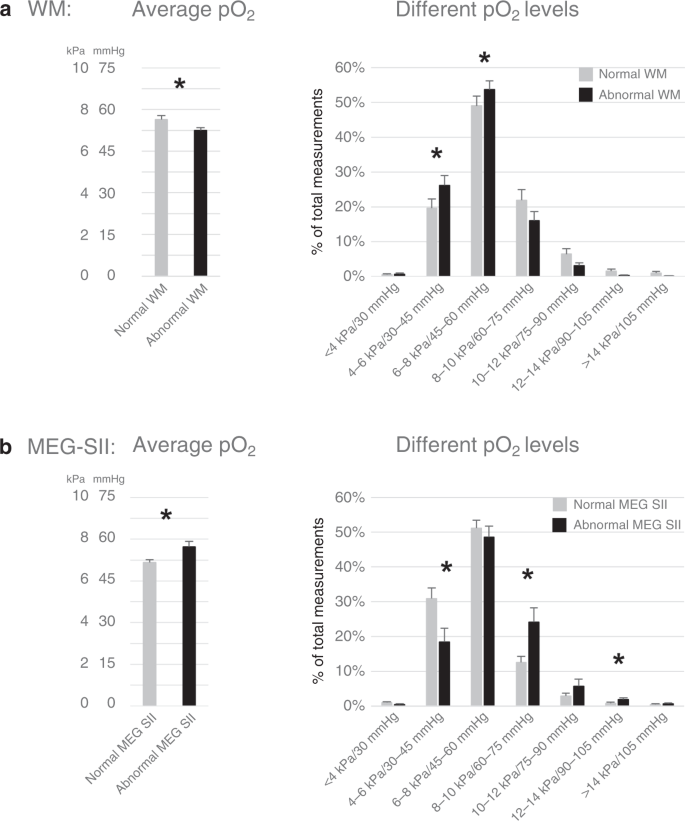
Arterial pO2 (averages and percentage of total measurements in subgroups; mean +/− SEM, *p < 0.05) during the outset 3 days of life in ELGANs a with normal (n = 43) or abnormal (n = 26) white thing (WM) and b with normal (n = 25) or aberrant (n = 14) Million-SII.
Patients with abnormal WM findings and major neurologic impairment in Hempel assessment (CP) had higher and patients with abnormal MEG-SII or low GMDS had lower demand for supplemental oxygen (FiOtwo)
The patients with WM abnormalities had spent more time (percentage of time) with supplemental oxygen (FiO2 >21%) and had required higher average FiO2 than the ones with normal WM (Fig. 4). The findings with astringent WM abnormalities were like (p < 0.01, DNS). Too the proportional times with FiO2 >30% (p < 0.01) and >lxx% (p < 0.05) were higher in infants with abnormal WM (Fig. 4c) and with severe WM outcomes (p < 0.01, DNS) than in those with normal WM. The ELGANs with major neurologic impairment in Hempel assessment (CP) too had a college need for FiO2, i.due east., they had college proportional times with FiO2 >lxx% (p < 0.01) and >90% (p < 0.05) than the ones with normal Hempel assessments (DNS).
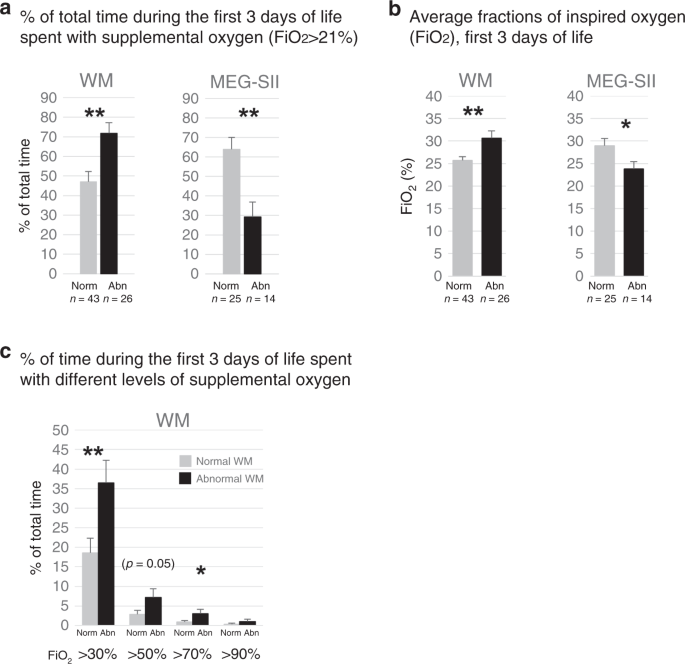
ELGANs with WM injury take higher and with aberrant One thousand thousand-SII lower need for FiOii than those with normal findings. a Time spent with FiO2 > 21% (%, mean +/− SEM); b average FiO2 (%, mean +/− SEM); and c per centum of fourth dimension (%, hateful +/− SEM) spent with unlike FiOii levels. *p < 0.05, **p < 0.01.
In turn, the infants with abnormal 1000000-SII had spent less time with supplemental oxygen and received less FiOii than the patients with normal Million-SII (Fig. 4a, b). Also the group with lower GMDS scores spent significantly less time with FiO2 >50% than the ones with better scores (p < 0.01; DNS).
To investigate the part of excessive oxygen administration, we analyzed the utilize of supplemental oxygen when the saturations were >95% or >98%. During the first iii days of life, the cumulative times when patients received supplemental oxygen while having SpOii >95% or >98% were not statistically significantly different betwixt any of the study groups (DNS).
Bradycardia (Hour <100 bpm) and low oxygen saturations (SpOii)
As bradycardia, in addition to oxygen-related factors, or in combination with hypoxia (apneas), is potentially associated with later neurodevelopmental impairments, we next studied the role of Hour, when being <100 bpm. During the outset 3 days of life, the ELGANs with WM abnormalities tended to accept more bradycardia than those with normal WM. In patients with abnormal and normal WM, the proportions of HR values <100 bpm relative to all HR values (per centum of total measurements) were 0.10 and 0.05% (p = 0.06), and the cumulative times (pct of fourth dimension during the first 3 days) when having HR <100 min were 0.18 and 0.15% (NS), respectively. The infants with abnormal WM tended also to suffer more from the combination of bradycardia and hypoxia as measured by the cumulative time (percentage of fourth dimension during the kickoff three days) when having 60 minutes <100 bpm and SpOtwo <85% (p = 0.05) or HR <100 bpm and SpOtwo <ninety% (n = 0.08) than the patients with normal WM (Fig. 5a). The differences betwixt normal and abnormal Meg-SII, Hempel, and GMDS (DQ) groups with HR data were non pregnant (DNS).
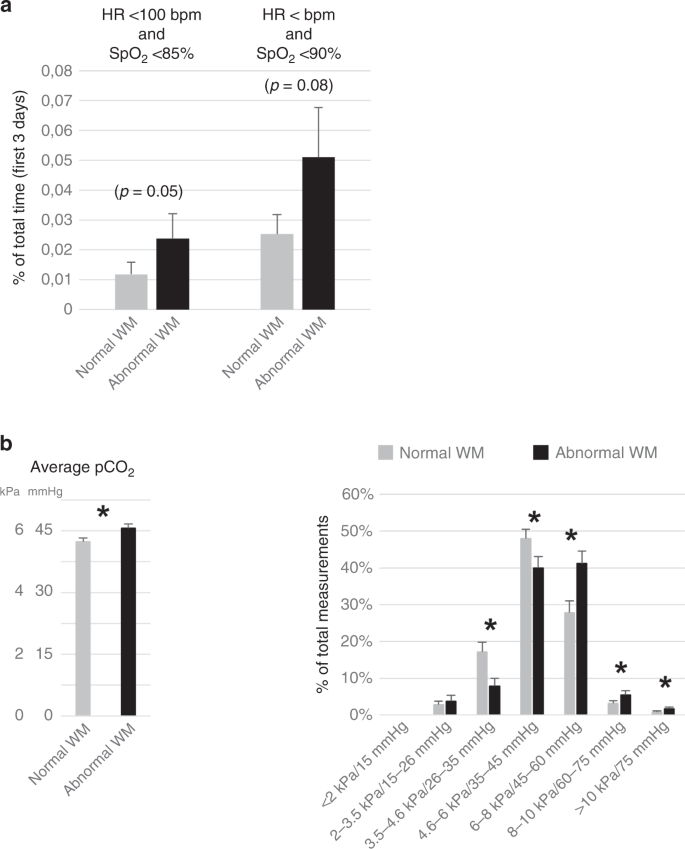
a Bradycardia (HR <100 bpm) and low oxygen saturations (SpO two ). Cumulative times, i.e., percentage of time (mean +/− SEM) during the commencement three days of life, when having at the same time eye rate (HR) below 100 bpm and SpOii < 85% or SpO2 < xc% in ELGANs with normal (northward = 43) or abnormal (n = 26) white matter (WM) in MRI at TEA. b Partial pressures of carbon dioxide (pCO2, arterial samples). Arterial pCOii (averages and percentage of total measurements in subgroups; mean +/− SEM, *p < 0.05) obtained during the showtime 3 days of life in ELGANs with normal (due north = 43) or abnormal (northward = 26) white matter (WM) in MRI at TEA.
Partial pressures of carbon dioxide in the written report groups
In arterial blood gas analysis, the infants with WM abnormalities had higher boilerplate levels of pCOii (Fig. 5b) than those with normal WM. Consistently, when analyzing unlike pCO2 levels, the patients with aberrant WM had more loftier level and fewer low level pCO2 values than those with normal WM (Fig. 5b). Regarding pCO2 levels, the patients with abnormal MEG-SII, low GMDS scores, or aberrant Hempel neurological examination did not statistically differ from those with normal findings (DNS).
Word
Due to advancements in neonatal intensive care and increased survival of ELGANs, the prediction and prevention of later complications accept go crucially important.4,5,six,7,eight,21,22,23 In the present study, nosotros demonstrate that the ELGANs with later WM abnormalities showroom lower really achieved SpO2 during their get-go iii days of life than the infants with normal WM. In turn, the results are different with infants having abnormal MEG-SII responses, who have higher early SpO2 than ELGANs with normal MEG-SII. We as well prove that both these abnormalities, i.e., severe WM changes and aberrant MEG-SII at TEA, correlate with adverse neurodevelopment at 2 years of corrected age. The role of WM injury in unfavorable development is in accordance with previous publications.8,17,20,21,22,23 The SII response, in turn, is considered every bit an indicator of college intracortical processing, and the absence of this response may reflect overall reduced corticocortical connectivity.19 The findings with WM and oxygen-linked factors are besides in agreement with previous studies showing relations between depression oxygen and WM injury,one,20,21,27 although hyperoxia has also been suggested to be harmful to WM.28 In terms of oxygen parameters and One thousand thousand-SII responses in infants, there are no previous information and the present findings are novel.
Consistent with the SpOii findings, the accomplished oxygen levels in arterial samples (pO2) in ELGANs with WM abnormalities were lower and with 1000000-SII and GMDS abnormalities higher than in their normal controls. Thus, despite technical, limit setting, and averaging challenges with pulse oximetry,14,29 and discontinuous information sampling with arterial pO2 levels, obtaining like results with both methods strengthens the results. The other limitations of the study include the number of patients, i.due east., although the amount of data from the database was big, the number of patients (final study population of 73 patients) may non have been powerful enough for discovering all clinically meaning factors. Furthermore, retrospective investigations ever take limitations. In terms of updates in later devices, we consider the data obtained from the monitoring devices of our study uniform, as, e.k., the limited setting and averaging challenges still exist with the updated pulse oximetry. The possible office of compliance with pre-established SpO2 ranges by the stuff was non determined, but one could presume that the potential effects of compliance would exist as targeted to all different groups and thus compliance would non explain the observed differences betwixt the patient groups.
The mechanisms underlying the opposite findings in early oxygen levels in patients with after WM injury and with abnormal One thousand thousand-SII responses are unclear. Only two of the patients had both abnormal WM and abnormal Meg-SII responses, whereas the others had either aberrant WM or MEG-SII. This suggests that the noxae causing these two conditions are probable to exist different. Indeed, certain jail cell types and tissue structures take been shown to exist more sensitive to hypoxia and others to hyperoxia. Hypoxia can, e.g., pb to proinflammatory and oxidative stress,1 increased production of hypoxia-inducible factors,30 and WM injury.21 Hyperoxia, in turn, has an impact on oxidative stress, changes in blood menses, disruption on neural plasticity and myelination, and may contribute to the encephalopathy of prematurity.i,28,31 Thus, the present results may bespeak certain brain structures being more vulnerable to hypoxia and others to higher oxygen levels.
The administration of supplemental oxygen (FiO2) seemed, at first glance, to have been clinically advisable, as the patients with lower SpO2 (abnormal WM) were supplied with higher FiOii and the patients with higher SpO2 (aberrant MEG-SII) with less supplemental oxygen (Fig. four). Moreover, the cumulative times of inappropriate oxygen assistants did not differ between the groups. However, the administration of appropriate FiO2 in the NICU may not have been dynamic enough as the really achieved oxygen saturations were relatively often out-of-the-target range (Fig. ii). Having said that, sure high SpO2 levels were not iatrogenically caused as some infants had high SpOtwo at room air, i.e., without supplementary oxygen. However, those occasions may yet have been harmful, as even at room air the oxygen exposure is higher than that encountered in corresponding fetal menstruation in utero.two,ten,32
Other than oxygen-associated factors are undoubtedly likely to be involved in causing neurological impairments in ELGANs. In the present study, the infants with WM abnormalities had lower Apgar scores, more RDS, BPD, and IVH, and thus seem to have been in more serious general condition during the NICU flow, than those with normal WM. Moreover, they were more often male, in whom the antioxidant defence maturation is shown to be delayed specifically when built-in preterm.32 All these factors may accept affected the later outcomes of these ELGANs. The SGA or twin infants, in turn, were not significantly overrepresented in the abnormal groups, only the written report is limited by the number of patients and may non have been powerful plenty to discover all clinically significant factors.
There are several additional factors that may play roles in inducing neurodevelopmental impairments in ELGANs. Indeed, in our report, the partial pressures of carbon dioxide in patients with abnormal WM were college than in those with normal WM. This is in accordance with previous studies showing the interest of hypercarbia and pCO2 fluctuations in agin neurological outcomes.33,34,35,36,37 Furthermore, vascularization and circulation are candidates for playing important roles. For example, vascularization of specific regions and the dissimilar regulation of vascular tone by oxygen and CO2 have been demonstrated with different regions of retina.38 Moreover, although in this study the findings with bradycardia (Hr <100 bpm ± low SpOtwo) did not reach statistical significance, there were trends, and apneas (low SpO2 and low 60 minutes) as well equally intermittent hypoxemia or hyperoxemia, systemic circulatory factors (e.g., Hr, blood pressure), and hemoglobin levels may play of import roles and need to be evaluated in the futurity. Additionally, we wish to correlate the early NICU information with the neurodevelopmental outcome at after ages, such every bit pre-school and school ages. Naturally, prospective investigations are needed to confirm the effects of early on oxygen parameters and other related factors in later neurodevelopment in ELGANs.
Conclusions
In decision, lower SpO2 and pOtwo levels and higher FiO2 need during the commencement 3 days of life in ELGANs associate with later on WM abnormalities and agin neurodevelopment. The infants with abnormal MEG-SII, which is associated with later low GMDS, bear witness the reverse findings, i.eastward., they have higher early SpO2 and pO2 levels, than the infants with more favorable MEG-SII and GMDS outcomes. The results indicate that of encephalon structures WM are more vulnerable to hypoxia, whereas others, such as cortical areas, are more sensitive to hyperoxia. Although the findings accept to be confirmed in further studies, they emphasize the importance of maintaining strict saturation targets during the early on postnatal flow.
References
-
Bakery, East. Chiliad., Jacobs, S. E., Lim, R., Wallace, Eastward. M. & Davis, P. G. Jail cell therapy for the preterm infant: hope and practicalities. Arch. Dis. Child. Fetal Neonatal Ed. 105, 563–568 (2020).
-
Andresen, J. H. & Saugstad, O. D. Oxygen metabolism and oxygenation of the newborn. Semin. Fetal Neonatal Med. 25, 101078 (2020).
-
Rogers, E. East. & Hintz, S. R. Early neurodevelopmental outcomes of extremely preterm infants. Semin. Perinatol. 40, 497–509 (2016).
-
Duncan, A. F. & Matthews, Grand. A. Neurodevelopmental outcomes in early babyhood. Clin. Perinatol. 45, 377–392 (2018).
-
Ream, Yard. A. & Lehwald, Fifty. Neurologic consequences of preterm nascency. Curr. Neurol. Neurosci. Rep. xviii, 48 (2018).
-
Marlow, Northward., Wolke, D., Bracewell, Grand. A. & Samara, Thou. EPICure Study Group. Neurologic and developmental disability at six years of age after extremely preterm nascency. North. Eng. J. Med. 352, 9–19 (2005).
-
Owen, L. Due south., Manley, B. J., Davis, P. Yard. & Doyle, Fifty. W. The evolution of modern respiratory care for preterm infants. Lancet 389, 1649–1659 (2017).
-
Hintz, S. R. et al. Neuroimaging and neurodevelopmental result in extremely preterm infants. Pediatrics 135, e32–e42 (2015).
-
Fiore, J. M. D. et al. Patterns of oxygenation, bloodshed, and growth status in the surfactant positive pressure level and oxygen trial accomplice. J. Pediatr. 186, 49.e1–56.e1 (2017).
-
Lui, G. et al. Lower versus higher oxygen concentrations titrated to target oxygen saturations during resuscitation of preterm infants at birth. Cochrane Database Syst. Rev. 5, CD010239 (2018).
-
Askie, Fifty. M. et al. Effects of targeting lower versus higher arterial oxygen saturations on death or inability in preterm infants. Cochrane Database Syst. Rev. 4, CD011190 (2017).
-
Schmidt, B., Whyte, R. K. & Roberts, R. South. Oxygen targeting in infants built-in extremely preterm who are small for gestational historic period: a need for heightened vigilance. J. Pediatr. 186, nine–10 (2017).
-
Kapadia, V. S. et al. Impact of the neonatal resuscitation program-recommended low oxygen strategy on outcomes of infants born preterm. J. Pediatr. 191, 35–41 (2017).
-
Cummings, J. J., Polin, R. A. & Committee on Fetus and Newborn. Oxygen targeting in extremely low birth weight infants. Pediatrics 138, e20161576 (2016).
-
Verhagen, Eastward. A. et al. Cognitive oxygenation is associated with neurodevelopmental outcome of preterm children at age ii to iii years. Dev. Med. Kid Neurol. 57, 449–455 (2015).
-
Saugstad, O. D. & Aune, D. Optimal oxygenation of extremely low birth weight infants: a meta-assay and systematic review of the oxygen saturation target studies. Neonatology 105, 55–63 (2014).
-
Woodward, 50. J., Anderson, P. J., Austin, N. C., Howard, K. & Inder, T. E. Neonatal MRI to predict neurodevelopmental outcomes in preterm infants. N. Eng. J. Med. 355, 685–694 (2006).
-
Rahkonen, P. et al. Cortical somatosensory processing measured by magnetoencephalography predicts neurodevelopment in extremely depression-gestational-age infants. Pediatr. Res. 73, 763–771 (2013).
-
Nevalainen, P. et al. Evaluation of somatosensory cortical processing in extremely preterm infants at term with MEG and EEG. Clin. Neurophysiol. 126, 275–283 (2015).
-
van Tilborg, E. et al. Impaired oligodendrocyte maturation in preterm infants: potential therapeutic targets. Prog. Neurobiol. 136, 28–49 (2016).
-
Dorsum, S. A. White matter injury in the preterm infant: pathology and mechanisms. Acta Neuropathol. 134, 331–349 (2017).
-
Arulkumaran, S. et al. MRI findings at term-corrected age and neurodevelopmental outcomes in a big accomplice of very preterm infants. AJNR Am. J. Neuroradiol. 41, 1509–1516 (2020).
-
Martinez-Biarge, Grand. et al. Neurodevelopmental outcomes in preterm infants with white matter injury using a new MRI classification. Neonatology 116, 227–235 (2019).
-
Hempel, Grand. S. The Neurological Exam for Toddler Historic period (University of Groningen, 1993).
-
Brandt, I. & Sticker, E. J. Griffiths Entwicklungsskalen zur Beurteilung der Entwicklung in den ersten beiden Lebensjahren (Beltz Test GMBH, 2001).
-
Rahkonen, P. et al. Atypical sensory processing is common in extremely low gestational age children. Acta Paediatr. 104, 522–528 (2015).
-
Juliano, C. et al. Mild intermittent hypoxemia in neonatal mice causes permanent neurofunctional deficit and white matter hypomyelination. Exp. Neurol. 264, 33–42 (2015).
-
Reich, B., Hoeber, D., Bendix, I. & Felderhoff-Mueser, U. Hyperoxia and the immature brain. Dev. Neurosci. 38, 311–330 (2016).
-
Lakshminrusimha, South., Manja, 5., Mathew, B. & Suresh, 1000. One thousand. Oxygen targeting in preterm infants: a physiological estimation. J. Perinatol. 35, 8–15 (2015).
-
Kalikstad, B., Kultima, H. G., Andersstuen, T. Grand., Klungland, A. & Isaksson, A. Factor expression profiles in preterm infants on continuous long-term oxygen therapy suggest reduced oxidative stress-dependent signaling during hypoxia. Mol. Med. Rep. 15, 1513–1526 (2017).
-
Panfoli, I. et al. Oxidative stress as a primary risk gene for brain damage in preterm newborns. Front. Pediatr. 6, 369 (2018).
-
Vento, M. et al. Antenatal steroids and antioxidant enzyme activeness in preterm infants: influence of gender and timing. Antioxid. Redox Point eleven, 2945–2955 (2009).
-
Dark-brown, M. K. et al. Incidence of hypocapnia, hypercapnia, and acidosis and the associated risk of adverse events in preterm neonates. Respir. Care 63, 943–949 (2018).
-
Dix, L. M. Fifty. et al. Carbon dioxide fluctuations are associated with changes in cerebral oxygenation and electrical activity in infants born preterm. J. Pediatr. 187, 66.e1–72.e1 (2017).
-
Leviton, A. et al. Newborn blood gas derangements of children born extremely preterm and neurocognitive dysfunctions at age 10 years. Respir. Physiol. Neurobiol. 242, 66–72 (2017).
-
Ambalavanan, N. et al. PaCO2 in surfactant, positive pressure, and oxygenation randomised trial (Back up). Arch. Dis. Child. Fetal Neonatal Ed. 100, F145–F149 (2015).
-
Molloy, East. J. & Cummins, E. P. Carbon dioxide as a drug in neonatology. Pediatr. Res. 39, 763 (2020).
-
Arduini, A. et al. Metabolic adaptation and neuroprotection differ in the retina and choroid in a piglet model of acute postnatal hypoxia. Pediatr. Res. 76, 127–134 (2014).
Acknowledgements
We are deeply indebted to Marita Suni, RN, for caring for the very prematurely built-in infants during the Million measurements. Nosotros also limited our gratitude to all our subjects and their families for preparing the style for this study. Finally, we give thanks the personnel of the maternity ward of the Department of Obstetrics and Gynecology and the Neonatal Intensive Care Unit at the Helsinki University Hospital and the neonatal ward at Jorvi Hospital for their cooperation. This study was supported by Päivikki and Sakari Sohlberg Foundation (to K.R.), Foundation for Pediatric Research in Republic of finland (to K.R., G.K., S.A.), Governmental Subsidy to Clinical Inquiry (to Southward.A.), Finska Läkaresällskapet (to S.A.), and Arvo and Lea Ylppö Foundation (to A.L.). The funding sources did not participate in the work.
Funding
Open admission funding provided by University of Helsinki including Helsinki Academy Fundamental Hospital.
Writer data
Affiliations
Contributions
Substantial contribution to the conception and blueprint: K.R., O.-P.R.-M., G.Thousand., J.H., S.S., M.J.50. and Due south.A. Conquering of data: K.R., O.-P.R.-K., M.One thousand., P.R., A.50., Fifty.L., and P.North. Analysis and interpretation of data: One thousand.R., O.-P.R.-K., M.G., J.H., S.S., P.R., A.L., Fifty.Fifty., P.Northward., M.J.50., and S.A. Drafting of manuscript: M.R. and O.-P.R.-K. All authors contributed to critical revisions of the manuscript and terminal approval of the version to be published.
Respective author
Ethics declarations
Competing interests
The authors declare no competing interests.
Consent statement
All parents provided signed informed consents.
Additional information
Publisher's note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Admission This article is licensed under a Creative Commons Attribution 4.0 International License, which permits apply, sharing, accommodation, distribution and reproduction in any medium or format, as long every bit y'all requite appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and signal if changes were made. The images or other third political party material in this article are included in the article'southward Creative Eatables license, unless indicated otherwise in a credit line to the textile. If cloth is not included in the article'due south Creative Commons license and your intended use is not permitted past statutory regulation or exceeds the permitted employ, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
Reprints and Permissions
About this article
Cite this article
Rantakari, 1000., Rinta-Koski, OP., Metsäranta, M. et al. Early oxygen levels contribute to brain injury in extremely preterm infants. Pediatr Res xc, 131–139 (2021). https://doi.org/ten.1038/s41390-021-01460-3
-
Received:
-
Revised:
-
Accepted:
-
Published:
-
Issue Date:
-
DOI : https://doi.org/10.1038/s41390-021-01460-three
Further reading
-
The twofold NICU claiming: avoiding hypoxia and hyperoxia
Pediatric Enquiry (2021)
Source: https://www.nature.com/articles/s41390-021-01460-3
0 Response to "Brain Damage in 9 Week Old Babies Due to Lack of Oxygen"
Post a Comment